Psoriasis- one of the most common diseases, the frequency of which in the population is constantly increasing every year. And if we consider that absolutely all age categories are susceptible to this pathology, and its simple form quickly enough flows into a more complex one, then the question of proper therapy and prevention is really very acute.
According to statistics, approximately every 30 inhabitant of the planet suffers from this ailment to one degree or another. What to do for those who get psoriasis? What medications and folk remedies can be treated? How to properly organize your meals? Let's finally put all the points.
Psoriasis and its causes
Psoriasis is an autoimmune disease with a rather vague etiology - the exact cause, despite numerous studies in this area, is still unknown. It is believed that this pathology is a consequence of genetically determined changes in the immune system, as a result of which chronic inflammation of the skin develops. However, its multifactorial nature is also not excluded - in other words, the involvement, along with heredity, and the influence of the external environment.
It is noteworthy that the predisposing factors, according to scientists, are quite different for different age groups: for example, if various types of bacterial infections, including, in particular, streptococcal infections, are considered to be triggering triggers in children, then for adults, stress stimuli and nicotine abuse are paramount. and alcohol, obesity, and the use of certain medications (eg, adrenaline receptor blockers).
It is impossible to completely cure psoriasis, however, modern medicine is quite capable of significantly alleviating the course of the disease and maintaining a long-term remission in the patient.
There are several theories to explain the onset of psoriasis:
- infectious and parasitic;
- neurogenic;
- endocrine;
- metabolic;
- immunological;
- hereditary;
- theory of molecular mimicry.
As with many other conditions, the cause of skin problems should be found in the gut. Its length is from 4 to 6 meters, and the inner surface is covered with villi, the total area of which is comparable to the size of a tennis court - this allows the absorption processes to proceed much more efficiently. Interestingly, the cells of the mucous membrane of the small intestine are completely renewed every 3-5 days. Here, moreover, up to 70% of human immunocytes are concentrated. So, one of the common causes of psoriasis is considered to be leaky gut syndrome (LEPS).
Deviation from the normal functioning of the intestinal mucosa is fraught with malabsorption, that is, a violation of the assimilation of basic nutrients (proteins, fats, carbohydrates, vitamins, minerals). In addition, the negative impact on the body of toxins and allergens increases: in such conditions, it is much easier for them to enter the bloodstream. The direct link between psoriasis and inflammatory bowel disease has been proven in numerous studies.
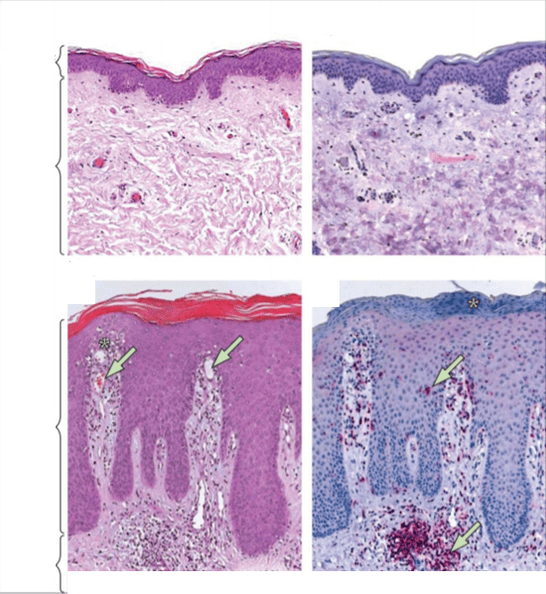
Other works of scientists confirm that a special microflora is formed on the skin of a patient with psoriasis, which is significantly different from the microbiome of healthy skin.
In the area of psoriatic lesions, a mass of various bacteria is concentrated, the stability of which is significantly lower than that of normal skin - in particular, colonization by Staphylococcus aureus is observed, which has an extremely negative effect on the course of the inflammatory process.
Types of psoriasis
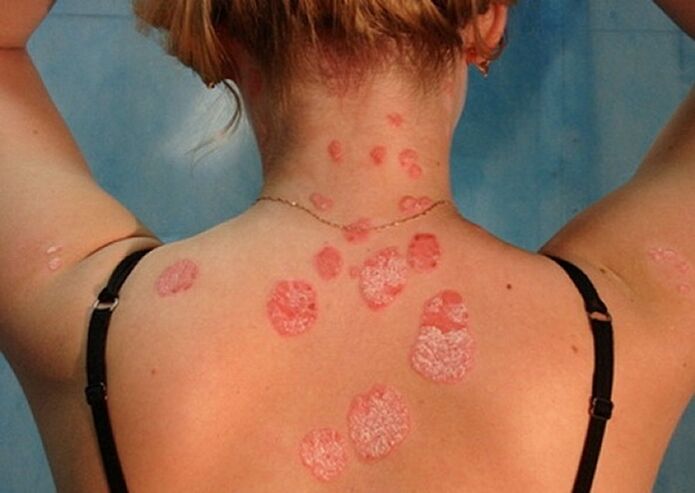
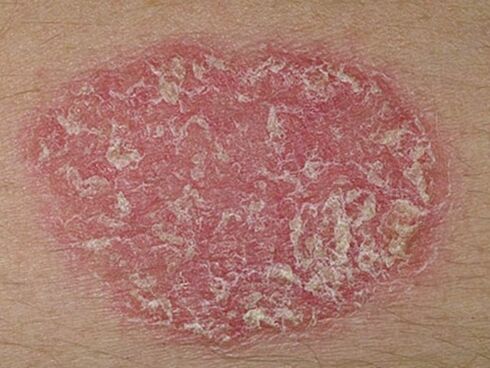
- Plaque psoriasis. . . In 90% of cases, dermatologists are faced with this particular form of the disease, also known as simple or ordinary. First, separate small areas appear on the skin, raised above the level of the healthy dermis. These inflamed areas are called psoriatic plaques. Gradually they grow, merging with neighboring spots into one whole.
- Reverse psoriasis.This diagnosis is given to patients who develop smooth red spots in the folds of the skin and inside the folds - in the groin area, on the inner thighs, under the breast. Unlike simple psoriasis, the foci of inflammation are practically not covered with scales, but due to their location and constant friction, they cause serious discomfort to patients. In addition, there is a danger of re-infection with streptococcus or fungus, since in places where spots are localized, due to high humidity and temperature, ideal conditions are created for the reproduction of microorganisms.
- Guttate psoriasis.This type of disease got its name from the shape of the formations. The lesions are in the form of a drop, raised above the level of healthy skin. A common trigger for this form of psoriasis is a previous streptococcal infection, as we mentioned earlier. The thing is that the patient's immunity, affected during the fight against the infection, is seriously weakened - his resources are not unlimited, and, like all living things, it takes time to recover - and it is against this background that an autoimmune disease is activated.
- Pustular psoriasis.It is considered the most severe form, accompanied by the formation of blisters filled with a clear liquid. Inflammation of the skin begins around the foci, swelling and thickening appear. With a secondary exacerbation, the likelihood of which is quite high, the blisters fill with pus. Localized foci of pustular psoriasis on the arms and legs. In difficult cases, there is a ubiquitous location of blisters on the body, their rapid growth and the danger of infection of the entire surface of the skin.
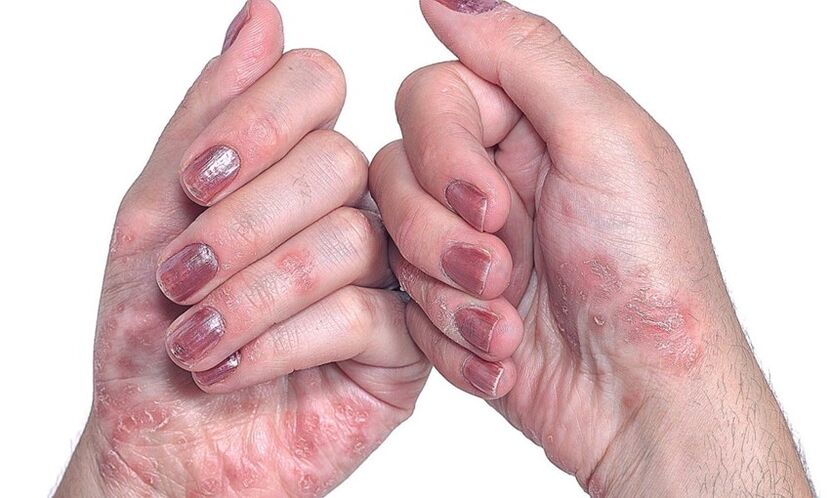
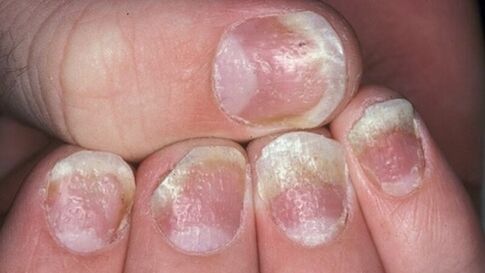
- Psoriasis on the nails.This type of disease changes the appearance and structure of the nail plates on the hands and feet. Nails thicken, lose their natural color, emit an unpleasant odor. The skin around the nail bed coarsens, thick ridges are formed. In advanced cases, the nails may disappear without subsequent regrowth.
- Psoriatic arthritis.In this case, the disease affects the joints and connective tissues. Most often, inflammation affects the distal phalanges of the extremities. There is psoriatic dactylitis - swelling of the fingers. The hip and knee joints are also exposed to the devastating effects of the ongoing disease. There are frequent cases of disability with loss of the ability to move independently.
- Psoriatic erythroderma.Flaky spots appear on the skin, while peeling of the affected layer is observed. Patients experience extreme discomfort due to constant itching and swelling. Most often, this diagnosis is made to patients who have already been treated for simple psoriasis, but have not completed therapy or have changed the drug.
Symptoms of the disease
The first manifestation of psoriasis is a small rash on the skin. Papules grow rapidly, growing to spots with a diameter of 4 to 8 cm, they become more and more, and dry scales form on the surface. In advanced cases, individual spots merge with each other, and the lesion affects large areas of the body. Psoriatic papules can be distinguished from other skin diseases by their round shape with clear boundaries, red or bright pink color, and silvery white scales. They appear first on those areas of the skin, the integrity of which is violated as a result of abrasions, wounds, frostbite, constant friction. There are three characteristic signs confirming the onset of the development of psoriasis:
- Stearin spot phenomenon- dry particles are easily separated from the affected surface, revealing an area that looks like a drop of wax or sterol.
- Psoriatic phenomenon(terminal) film. Further cleansing the papules from scales allows you to see a transparent and moist film, the skin under which is inflamed.
- Auspitz Phenomenon. . . Removal of the terminal film leads to the appearance of the smallest drops of blood on the surface of the stain.
This triad of psoriasis is unique - its presence allows the correct diagnosis to be made unmistakably. Nevertheless, different parts of the body have their own characteristics of the manifestation of the disease.
- Psoriasis on the body.The back, neck, abdomen, thighs and lower legs are most often affected by guttate psoriasis. Small papules, which resemble drops in shape, gradually grow, rising above the surface of the skin. This form of the disease is often diagnosed in people who have had a staphylococcal infection.
- Psoriasis on the hands.The most common places for the appearance of psoriatic papules on the hands are the elbows and interdigital spaces - while, as a rule, a plaque form is observed, in which individual small fragments merge into a single lesion area covered with dry scales. The forearms are much less likely to be affected.
- Psoriasis on the legs.The disease begins with single rashes in the knee area. Inflamed areas disturb patients with severe peeling and itching, quickly increase in size and merge with neighboring ones.
- On the palms and feet.In most cases, the simultaneous defeat of both the palms and the feet is recorded, but in some patients the ailment affects the stratum corneum of the purely upper or lower extremities. As a result of the growth of psoriatic papules, thickening, coarsening of the skin occurs with further cracking.
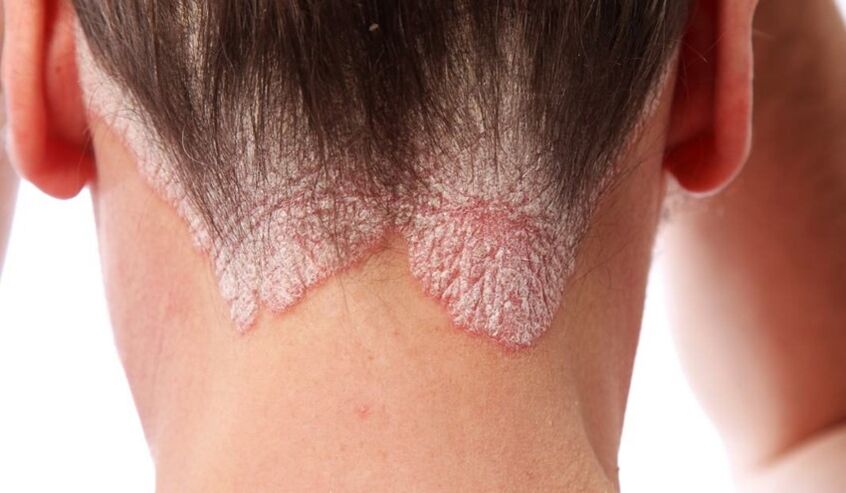
- Psoriasis of the scalp.First of all, rashes appear in the forehead, back of the head, and also behind the ears. First, patients note in themselves single scaly formations that grow, merge with those located nearby and, over time, can affect the entire scalp. Papules are very itchy, causing, thereby, a constant desire to scratch the skin - the resulting wounds and cracks are likely to become the entrance gate of infection. Dry particles are separated from the damaging formations - first small, somewhat similar to dandruff, and then larger flakes.
- On the face, ears, neck.Localization of psoriatic papules on the face is rather an exception in the usual clinical picture. In rare cases, when this does happen, the ailment affects the areas around the eyes and eyelids, as well as the cheeks and tongue. Formations on the neck quickly spread further - to the back or head. Ears are the site of development of seborrheic psoriasis. Papules can appear both inside the cartilaginous shell and outside. When making a diagnosis, it is important not to confuse the disease with seborrheic eczema, which has similar symptoms.
- On the nails.There are three options for the initial manifestation of psoriasis on the nail plates. The first is the emergence of small punctate depressions. The second is a thickening of the nails, a change in their natural color to gray or yellow. With the further development of nail psoriasis, the plate exfoliates, the upper particles are easily separated. And, finally, the third is a deformation of the nail, accompanied by a loss of smoothness by the plate and the appearance of depressed areas.
- Symptoms of psoriasis in children.At an early age, the disease proceeds differently: the main localization of red scaly rashes is skin folds: inguinal, in the elbow and popliteal folds, on the neck. Papules itch a lot, children experience constant torment, become irritable and restless. In general, all clinical variants observed in children are similar to those observed in adults. The differences concern purely manifestations, the location of the pathological process and the course of the disease itself.
4 stages of psoriasis
Clinical dermatology, based on differences in symptoms, degree of skin lesions and duration, distinguishes three stages of the course of psoriasis. However, there is an opinion that the initial stage must be recognized as another full-fledged stage in the development of the disease.
- Initial stage.The first sign of psoriatic lesions are small rashes. The places of their appearance can be different and depend on the type of disease. Primary papules are no more than 3 mm in size, painted in a pale pink color, which after 3-4 days is replaced by a gray bloom - dead dermis particles form on the spot. This process is accompanied by itching and burning, and the general health worsens. In general, the formation of plaques at the initial stage takes up to three weeks, and at this time a person has a chance to slow down the development of pathology.
- Progressive.At this stage, the ailment affects large areas of the skin: for example, with ordinary psoriasis, plaques are formed, with other forms - papules characteristic of them. In the process of development of the disease, individual spots merge with each other, covered with gray scales. The symptom by which the progressive stage is determined is the Köbner phenomenon (isomorphic reaction). Any damage to the skin after a while is accompanied by the appearance of a psoriasis rash in this place. Another confirmation that the disease is actively developing is the appearance of drops of blood, similar to dew, after removal of the plaque. The duration of this stage depends on the type of lesion. On average, it takes from two weeks to two months.
- Stationary stage.During this period, a thick grayish-white or gray crust forms. The pink rims disappear. The skin becomes rough, dry particles are constantly exfoliated from it. The itching and burning sensation becomes less annoying, but it also does not go away completely. New papules are not formed. This stage can be quite lengthy.
- Regressive stage.The final stage of the development of the disease, during which there is a gradual reduction and resorption of plaques. Itching no longer bothers. A clear sign of regression is Voronov's symptom, when papules are surrounded by white rings. The fading of spots occurs from the center to the periphery, as a result of which bizarre patterns form on the skin. By the end of the regressive stage, only areas of the skin that are slightly different in shade from healthy areas are reminiscent of psoriasis. There is no need to talk about complete recovery in the case of psoriasis. The end of the regressive stage indicates that the cycle of the disease is completed, which can return at any time. In order for remission to be prolonged, it is necessary to pay attention to health: avoid provoking factors, follow a diet, be observed by a dermatologist.
Examination plan for psoriasis
- General clinical analysis of blood.
- Research on the content of vitamins D, B12, folic acid in the blood.
- Blood test for ALT (alanine aminotransferase), AST (aspartate aminotransferase), direct bilirubin, alkaline phosphatase, gamma-glutamyl transferase, cholesterol with a lipid profile, creatinine, glucose, insulin, total protein.
- Blood for rheumatoid factor, c-reactive protein, uric acid, ASLO.
- Ferritin, transferrin, serum iron are indicators of anemia (in particular, chronic diseases).
- Thyroid panel: TSH, T4 sv, TK sv.
- Coprogram.
- KhMS according to Osipov.
- Ultrasound of the abdominal organs.
Traditional treatments for psoriasis
Early therapy.
The sooner a person who has discovered the first signs of skin lesions see a doctor, the more chances are to take timely measures that will prevent the rapid development of the disease and its transition to a chronic form - and, therefore, will significantly improve the overall standard of living.

One of the most commonly prescribed drugs at the onset of the disease is salicylic ointment. It has an anti-inflammatory and antimicrobial effect, has a keratolytic effect, due to which plaques are cleared of keratinized particles. To reduce itching, naphthalan ointment is also used.
Therapy at a progressive stage.
At this stage, an integrated approach to treatment is required, and only an experienced specialist can provide it. Treatment is aimed at relieving symptoms, ridding the body of toxins. To normalize metabolic processes, intramuscular injections of calcium gluconate are often prescribed. Sodium thiosulfate relieves inflammation and eliminates the manifestations of intoxication.
To moisturize the inflamed skin, special emulsions and salicylic ointment are used. Means containing tar are contraindicated at a progressive stage: they act irritating and increase the suffering of the patient.
When the intensity of inflammation decreases, physiotherapy procedures can be connected. Patients with psoriasis are shown ultraviolet irradiation, PUVA therapy and paraffin applications. Corticosteroids and cytostatics are not used unnecessarily, these potent drugs are needed exclusively in difficult and advanced cases.
To reduce allergic manifestations, antihistamines are prescribed, and sedatives are prescribed to reduce nervousness. Diuretics help reduce swelling of inflamed skin and remove toxins from the body.
Stationary therapy.
At this stage, the inflammation fades away, the plaques become covered with a dry crust, therefore, funds are needed that will alleviate the discomfort from the appearance of scales. These are tar shampoos, oil-based emulsions.
In many patients, ultraviolet irradiation and the PUVA technique have a good effect. If there is no improvement, doctors prescribe cytostatics.
Therapy at a regressive stage.
In the final period of the disease cycle, a constant correction of treatment methods is required, depending on the current state of the patient. Prevention is replacing active therapeutic actions.
The patient receives recommendations for changing the diet and lifestyle in general. In order to avoid the return of the skin lesion, it is necessary to avoid stressful situations that trigger the formation of psoriatic plaques.
Typically, doctors give patients the following advice:
- reconsider lifestyle: make adjustments to the diet, get enough sleep, move more;
- ensure normal vitamin levelsD, iron, B vitamins, protein in the body;
- normalize the digestive tract: exclude hypoacidity, impaired outflow of bile, SIBO and CIGR (syndromes of excessive bacterial and, accordingly, fungal growth);
- get rid of foci of chronic infection: sanitize the oral cavity, undergo treatment with an ENT doctor;
- deal with concomitant somatic pathology: hypofunction of the thyroid gland, insulin resistance, metabolic syndrome, etc.
Traditional methods of getting rid of psoriasis
- Initial stage.At the first sign of skin lesions, juniper and lavender oils are effective. They soothe irritated areas of the dermis, promote healing of minor injuries, relieve the feeling of tightness. A few drops of oil are added to a cream that is neutral in composition, for example for children, and applied to the rash that appears. Another popular method of dealing with the initial manifestations of psoriasis is the use of 3 percent hydrogen peroxide. Any measures, even the most harmless at first glance, can be applied after consulting a dermatologist. Diet changes, avoiding unhealthy foods and alcohol are also common recommendations of traditional healers.
- Progressive stage.At the stage of the rapid development of the disease, an infusion of celandine is added to the healing oils and hydrogen peroxide. To prepare it, you will need fresh or dried plant stems and salt water. Alcoholic tinctures are contraindicated, they can worsen the condition of the affected skin. It is necessary to insist celandine for at least several hours, and before applying the healing solution to the plaques, treat them with birch tar.
- Stationary stage.At the stage of termination of the formation of new papules, you can use proven folk methods that will definitely not harm the patient. These include the use of sulfuric ointment, salicylic solution.
- Regressive stage.At the final stage of the course of the disease, hirudotherapy (leech therapy) is often used. Although this method is not officially recognized by traditional medicine, many experts do not rule out its effectiveness. The procedures are carried out within 3 - 10 days, depending on the patient's state of health.

Prevention of psoriasis: how to prevent the development of the disease
- Skin care.To minimize the likelihood of psoriatic damage in the presence of a genetic predisposition, simple ways to maintain skin health will help: water and hardening procedures (bathing in the sea, baths with herbal extracts and salts, contrast showers, dousing with cool water in the air, etc. ); using soft sponges and avoiding hard washcloths that can damage the skin; the use of detergents, natural in composition, without aggressive chemical components.
- Ultra-violet rays.Several studies have proven the beneficial effect of sun exposure on the skin prone to psoriatic plaque formation. Moderate doses of ultraviolet light help accelerate tissue regeneration and reduce inflammation. You should not abuse sunbathing: an excess of rays can provoke an exacerbation of the disease.
- Clothing.Synthetic fabrics, tight-fitting styles, an abundance of belts and fasteners - all this is contraindicated for patients with psoriasis, even in remission. Clothing should be natural, hypoallergenic, loose, not causing any inconvenience that can lead to the return of pronounced symptoms. Dark tones should be avoided for aesthetic reasons; silvery white scales are less visible on light-colored garments.
- Injuries.For patients with psoriasis, any small wound, scratch, abrasion can cause the return of the progressive stage and secondary infection of the skin. They should be extremely careful to avoid injury.
- Cosmetic and household products.Not all remedies are suitable for maintaining cleanliness for people with such diagnoses. When choosing shower gels, soaps, shampoos, it is important to pay attention to their composition, giving preference to those that contain natural ingredients. It is better to purchase therapeutic series of care products that are sold in pharmacies. Scrubs with solid particles are absolutely contraindicated: they are able to start the process of the disease again due to the smallest injuries on the skin. Household chemicals should also be selected based on health safety; do not use aggressive cleaning powders based on chlorine and alkalis. Gloves should be worn when cleaning to avoid negative effects on the skin of the hands.
- Vitamin therapy.Maintaining the balance of vitamins is indicated for everyone, and especially for people with chronic dermatitis. Complex preparations keep the body in good condition, help it resist viruses and prevent metabolic disorders.

Psoriasis- this is not a death sentence, but a very serious reason to reconsider the rules by which you lived before. Your allies on the path of taming the disease should be competent professionals - dermatologists, nutritionists, therapists. With their help, as well as through a deliberate approach to treatment, you can learn to live comfortably, despite your diagnosis.























